
As a reminder, providers must be registered with Medicaid to serve members enrolled in Platino Plans. To avoid payment denials, enroll with Medicaid by visiting the Provider Enrollment Portal (PEP): medicaid.pr.gov/Home/PEP.
For questions or assistance, contact the EMPR/Envolve Vision team at (800) 531-2818.
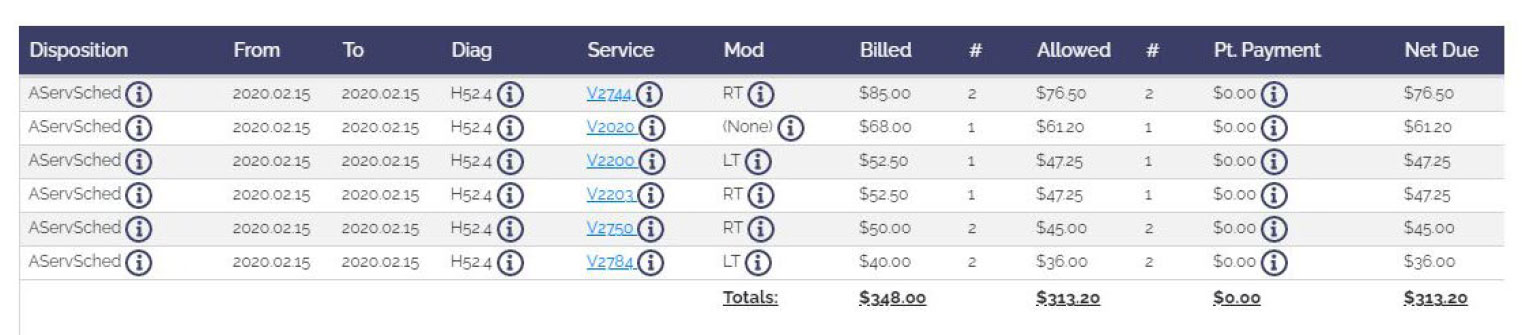
When billing for ophthalmic hardware, providers must report HCPCS codes in alignment with the frame, lenses and lens add-ons provided. Combining all charges under one code (V2020) will skew billing profiles and may result in unnecessary chart audits to review billing patterns.
To avoid this scenario, bill each item separately with the appropriate HCPCS code. Include the actual office cost as it is shown on the member’s receipt. This will help members better understand costs and reduce overbilling complaints.
In the example below, the office is billing for frames, polycarbonate lenses, transition lenses, bifocals, and anti-reflective lenses. Making this small change will help members better understand their benefits.
For your convenience, all eligible ICD codes can be found on Envolve Vision’s website at
Eye Management of Puerto Rico (EMPR) and Envolve Vision Benefits of Puerto Rico (Envolve Vision) are committed to improving the health of the communities we serve by helping people with diabetes lead healthier lives. Because of your vital role in patient health, we ask for your assistance in facilitating preventive care through annual diabetic eye exams and reporting of exam findings. Routine retinal evaluation is recommended to reduce the risk of diabetes-related blindness.
Please remember that 3072F should be included in your claim filing to indicate no evidence of diabetic retinopathy in the prior year, when applicable. For questions regarding diabetic care coordination, contact Envolve Vision’s Customer Service at the appropriate number below.
MMM: (844) 833-1905
MCS: (855) 754-4943
Please verify that your office information is up-to-date – including office hours or contact information that may have recently changed. There are three convenient methods to update your contact information:
Envolve Vision offers a Provider Education page for your convenience. Click below for:
Envolve Vision Proudly Serves. . .
All eye doctors are re-credentialed every 36 months unless otherwise requested by the payor. Reminder notices are distributed three months and one month prior to the expiration of the eye doctor's credentials. Anyone who fails to re-credential may be terminated from our provider panel for any applicable products. PROSHA Certificate and PRMMIS IDs are required a time of re-credentialing.

Unless otherwise stated in the Plan Specifics (found in the Eye Health Manager at envolvevision.com/logon), providers have these options to submit claims to Envolve Vision via the following:
Envolve Vision strongly encourages verifying member eligibility prior to rendering services. Providers may verify eligibility through Eye Health Manager at envolvevision.com/logon or call Envolve Vision’s Customer Service at:
MMM: (844) 833-1905
MCS: (855) 754-4943

For more than 30 years, Envolve Vision has partnered with vision care providers across the country to administer eye care programs that meet the needs of their members. You are among 22,000+ unique eye care providers, including independent providers and popular retail chains, within our network. Thank you for partnering with us to provide quality vision services to your patients.
